What I learned from a pelvic floor therapist about the importance of taking good care of our pelvic floor.
I recently had the opportunity to meet Brittney Davis, a pelvic floor specialist at Rock Valley Physical Therapy here in North Liberty, Iowa. Our initial meeting stemmed from a maternity project I recently completed. I quickly learned that care of the pelvic floor goes way beyond those who are currently pregnant or have ever carried a child.
Pelvic care has become a more significant part of the natal and post-partum care conversation, but as it turns out, a weak pelvic floor can affect men as well as all women!
Any chronic pressure on the pelvic floor can affect how strong our pelvic floor will be as we age. I was surprised to learn many of our “normal” habits and things we consume could be causing issues with our bladder and colon, affecting the pelvic floor. We ignore many of the indicators of problems because no one told us these are symptoms that could result in problems in our later years. A few of those signs are the inability to hold a fart, feeling frequent urgency to pee, being constipated, or having chronic loose bowels. These indicators could lead to problems such as rectal prolapse, incontinence, and erectile dysfunction in men.
Of course, I brought my pelvis illustrations with me when I met with Brittney to get the input of a specialist, and I am delighted to report that she found them very well done and well-researched. This was important to me because while I was researching the pelvis and trying to create something understandable of the web of muscles, ligaments, and tendons, I quickly learned that most women, myself included, only knew an area hurt. There was no name for the location – just an indicator of pain. I used this information to learn what pains women often experience, what the pain felt like, and interpreted the best-associated muscle. While my illustrations do not show every single muscle in the pelvic floor, I have illustrated and annotated the most significant regarding pain and strengthening.
The pelvic floor for the post-partum woman:
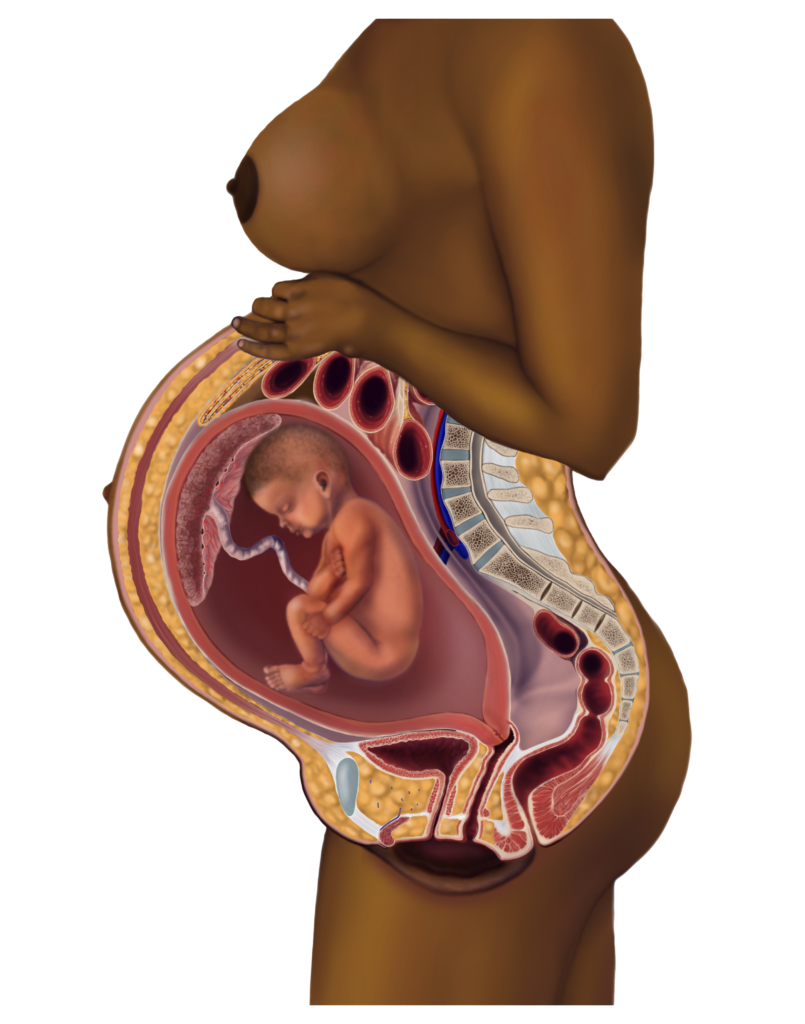
Let’s start where we know the pelvic floor has suffered trauma and why I created these illustrations – pregnancy.
Whether it was a vaginal birth or a c-section, the pelvic floor has had to support a significant accumulating weight for over 9 months! Like any other part of the body, that means there is wear and literal tear. Brittney supports a 2-week post-partum check-in to start new mothers on recovery – the sooner you start, the better. This is the time to check how the vulva and vagina are healing and check for diastasis recti abdominous (DRA) – the separation of the abdominal muscles.
The 6-week check-in is to check scars: test mobility and begin vaginal stretching. Brittney emphasized the importance of having a therapist help with vaginal stretching rather than a significant other because of the psychological response that could significantly affect future intimacy, highlighting the importance of proper care of a mother’s body to make sure an individual continues having the best quality of life including protecting their mental health.
Check-ups include advising cognitive load, tips on nutrition, and additional information on hormonal effects like breastfeeding. If a new mother is breastfeeding, the relaxin can increase joint mobility, causing pelvic pain and increasing the potential of an injury. These hormone changes can also cause anxiety and reduce an individual’s spatial awareness, making them more accident-prone. Loose joints and accidents are a fast and avoidable trip to the hospital!
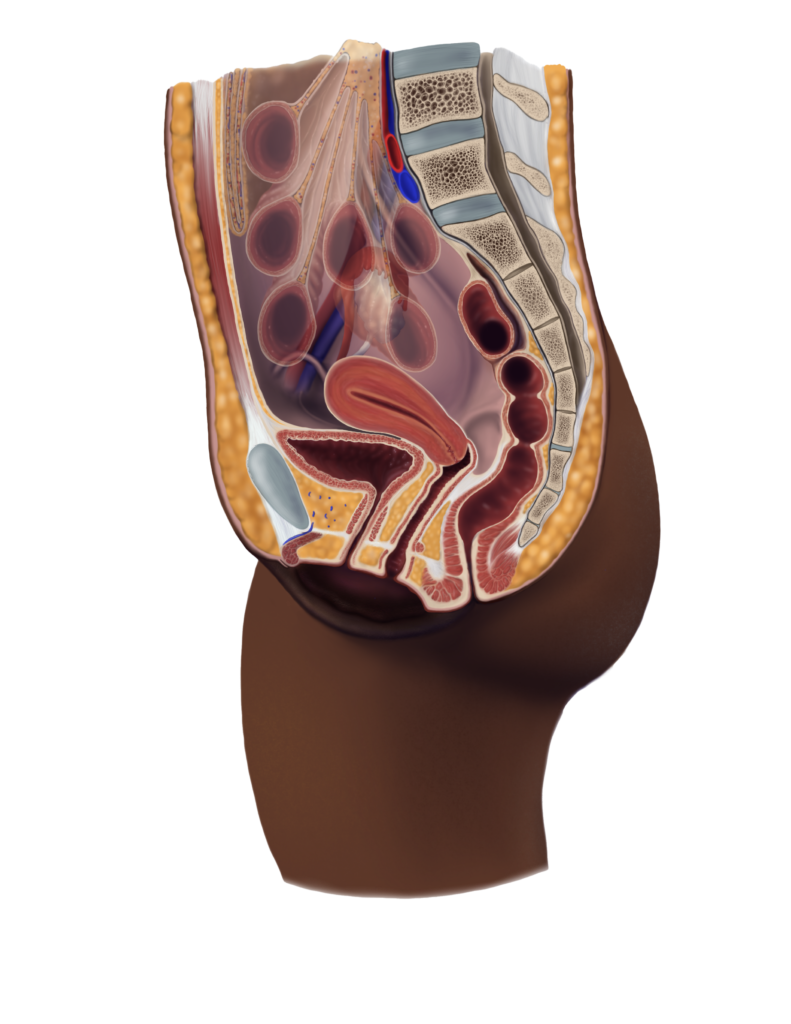
Not every woman gives birth – but what about menopause?
As we get older, we lose muscle tone and skin elasticity. Our skin loses its plumpness; with that, we can lose our ability to hold our pee. The number of women who are dependent on their tissues to help their sphincters hold steady is staggering, and things like office jobs and sitting with poor posture can slowly damage our pelvic floor.
A physical therapist like Brittney can teach better posture and help develop good stretching habits to save your urethra’s sphincter in the future.
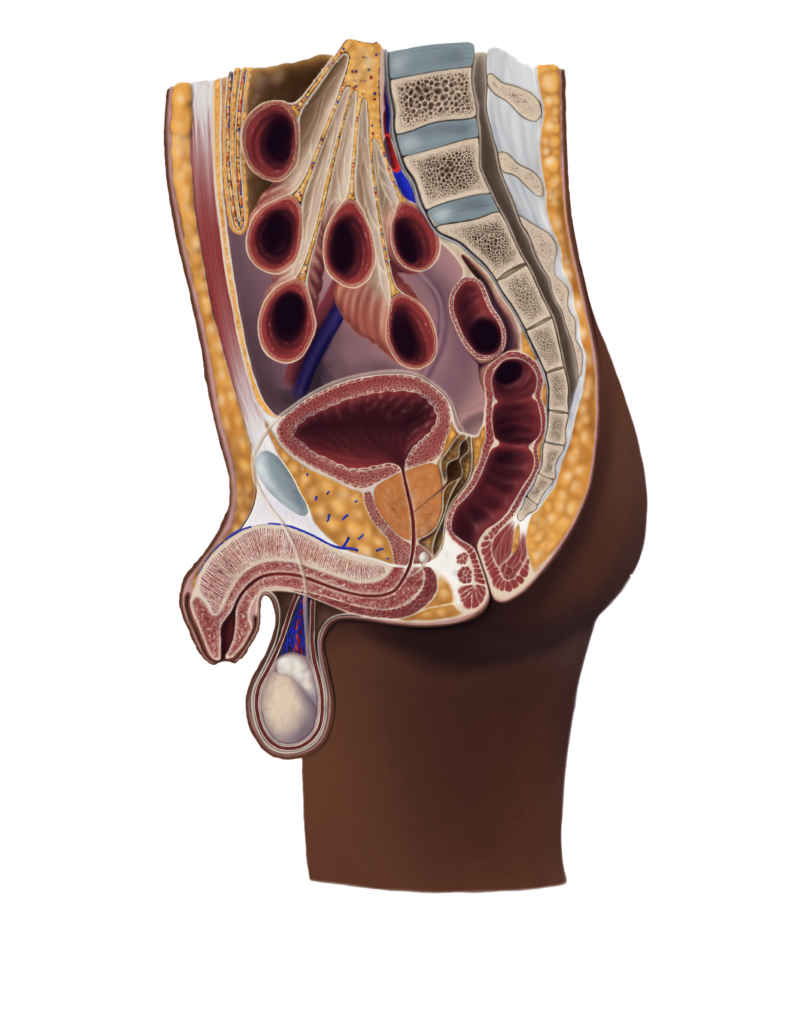
Men too?
Men can also have a damaged or weakened pelvic floor due to poor bowel habits, obesity, prostate surgery, or even repeated poor form when lifting heaving things. They can also develop bladder and bowel incontinence and erectile dysfunction.
Like exercising our hearts with cardio or lifting weights to build strong muscle and bone, we must also develop healthy habits to keep a solid pelvic floor.
Practice healthy eating habits to support regular bowel movements, learn proper bathroom form, and practice better posture. These little habits can help prevent problems, but when you feel pain – go to a physical therapist.
I urge all of us to start talking.
Talk about your pelvic discomfort, painful sex, and bowel habits. Part of the reason people are just living with their pain is because we have normalized it. We tell women to “try to relax” or “have a glass of wine.” Many things like this are chalked up to aging when they could have been helped or prevented.
Talking with Brittney opened my eyes to how much we neglect one of the most essential parts of our body – the part that helps bring life into the world, keeps us mobile, and keeps us comfortable and confident as we go through life.
Could a pelvic floor specialist be for you?
Brittney’s expertise on women’s health and pelvic floor care urged me to tell every woman I know (pregnant or not) to consider googling pelvic floor specialists in their area (and there are many!) and consider going to a pelvic floor therapist to enjoy the freedom of a strong pelvic floor.
While Brittney does her job helping people, my illustrations help professionals like Brittney better serve their clients by aiding pelvic floor education, increasing care, and self-advocacy.

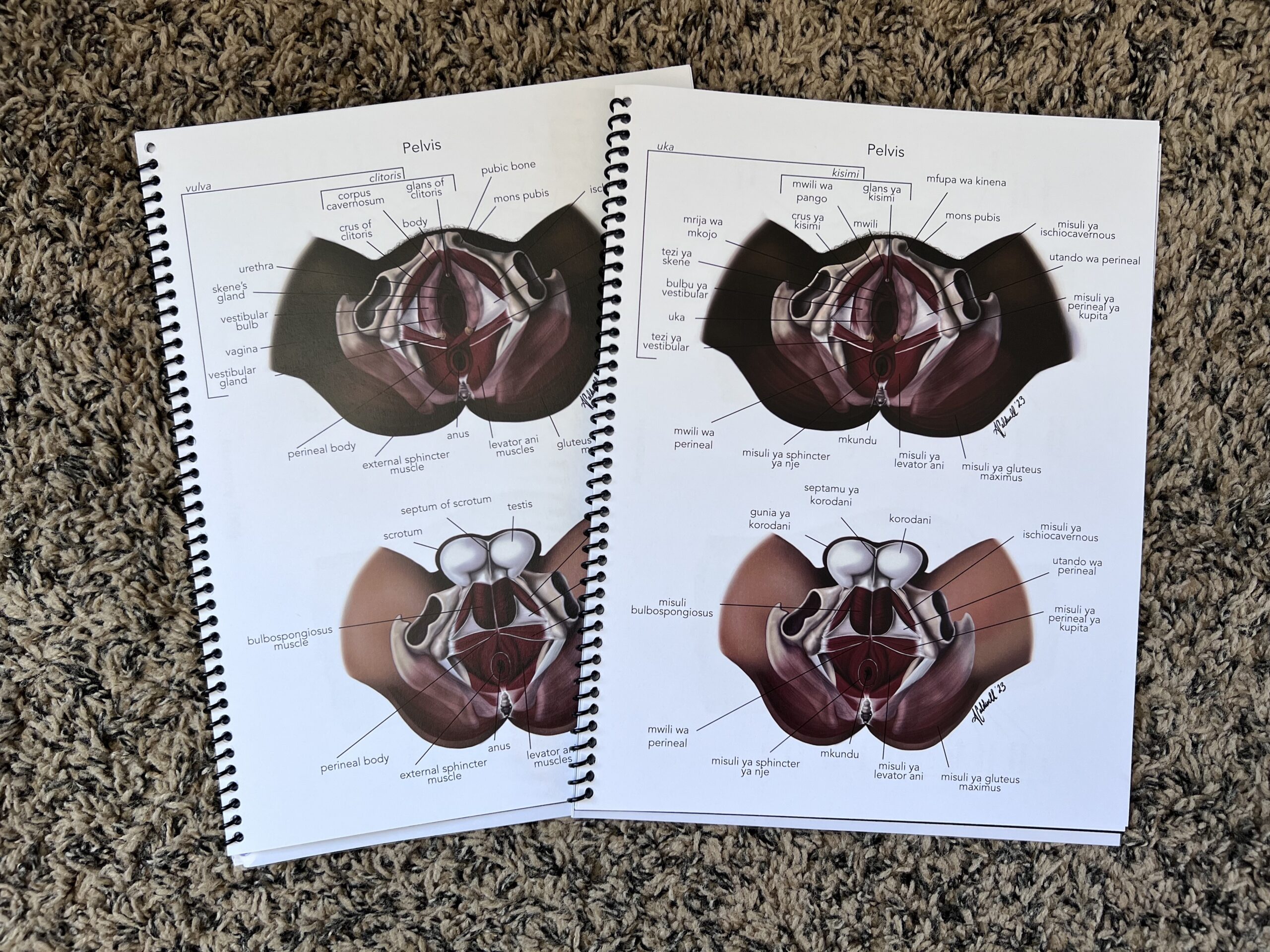
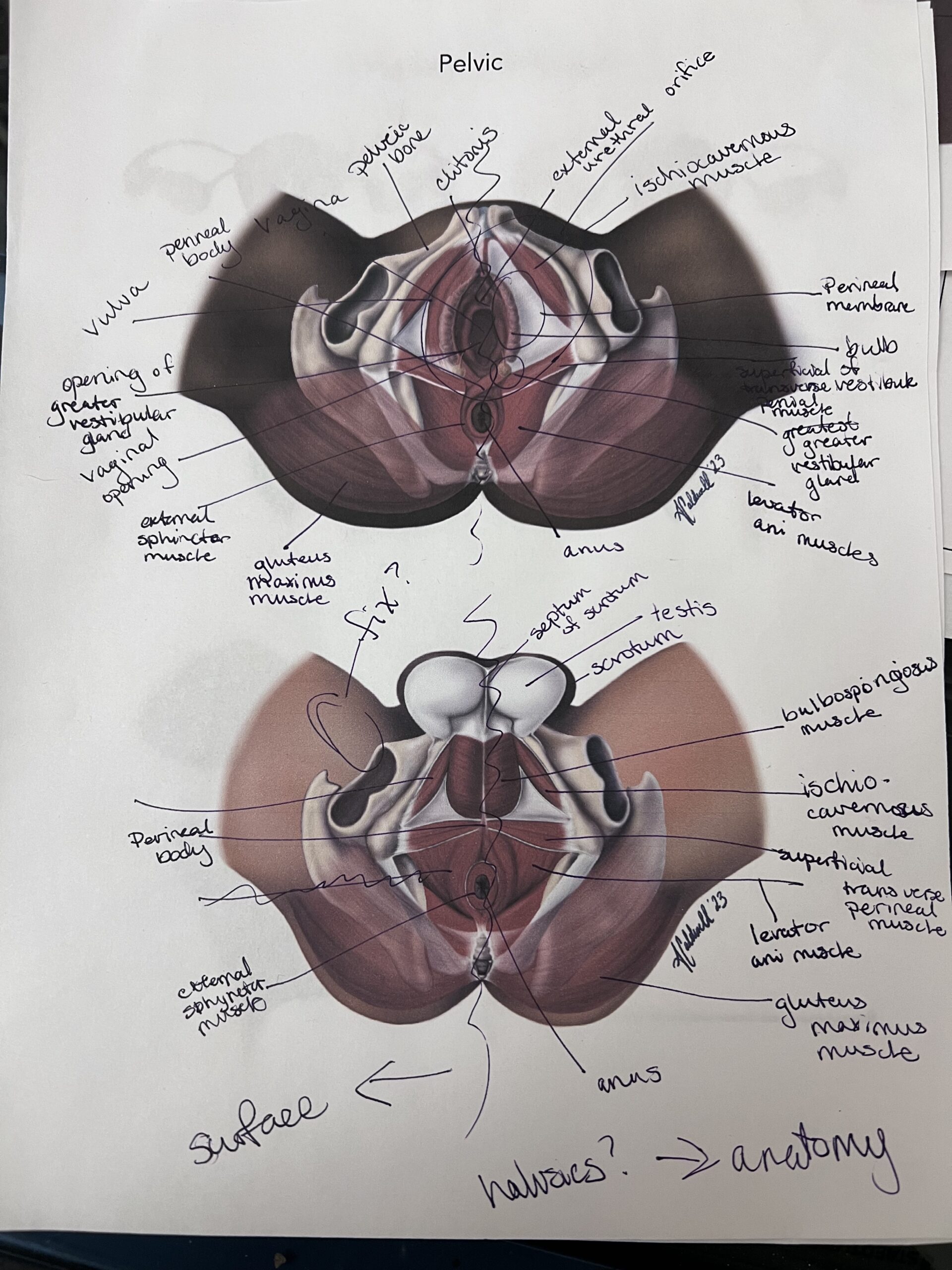
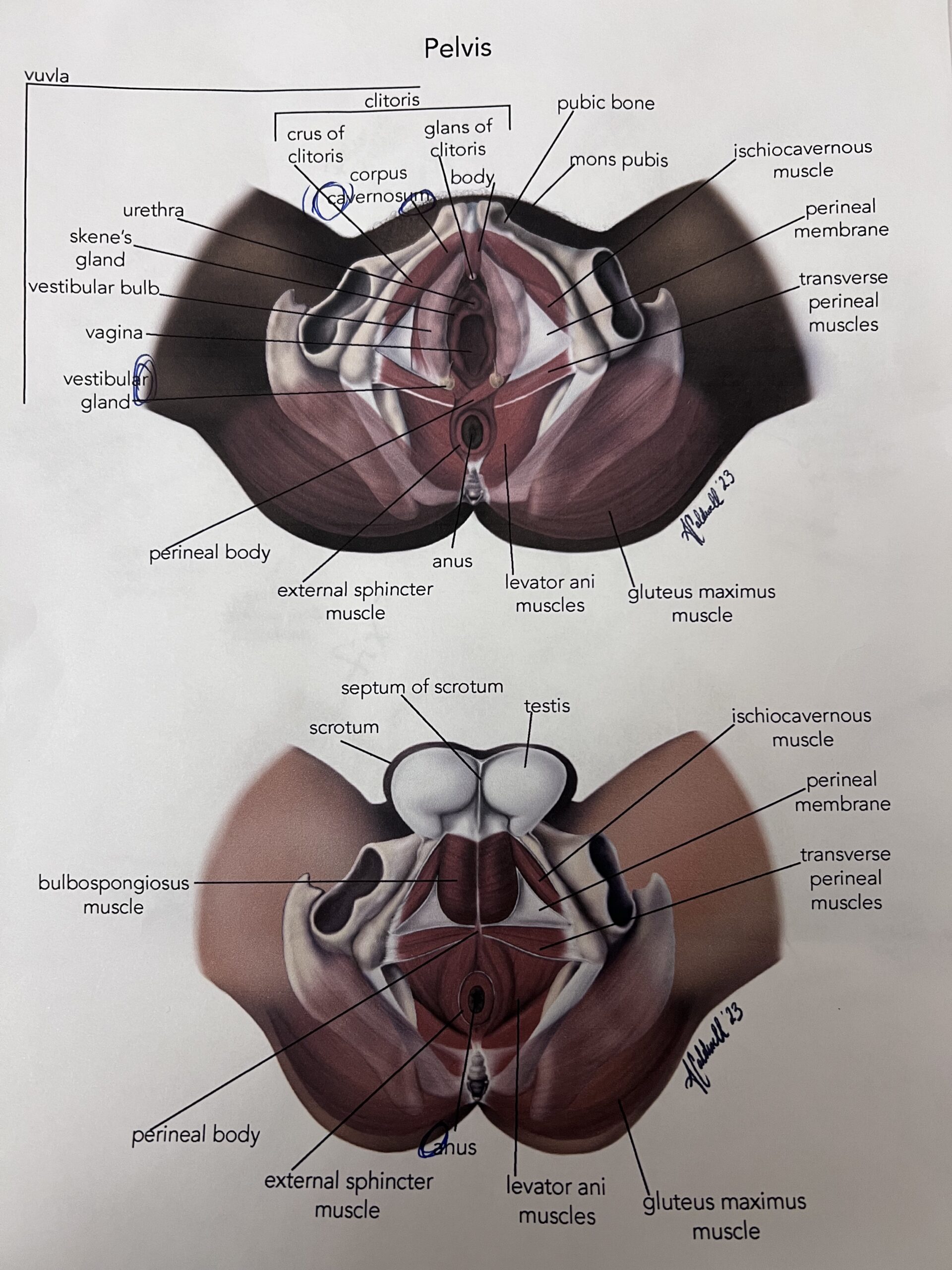
Great illustration and explanation of the importance of the pelvic floor muscles. Having worked in the pelvic health physiotherapy department, I have often advised pregnant and post -partum patients how to do the exercise and explain the importance of continued strengthening of these muscles into their lifestyle like any other exercise. It is good to know about pelvic floor exercise for all women regardless if they decide to have children or not.